“Strain” is the term given to a full or partial tear of the muscle fibres, muscle fascia (a.k.a. myofascia) or tendons – basically anything to do with the muscular structure.

This is different from a “sprain” which is a tear injury to the ligaments or joint capsules, which are types of tissue different to muscles.
It is also different from a “pulled” or “twinged” muscle, which is a muscle in spasm.
Very briefly:
- Tendons attach muscles to bones; a tear injury is called a strain.
- Ligaments attach bones to bones; a tear injury is called a sprain.
To understand the definitions better, we need to learn what the words mean. (If you just want to skip the boring definition stuff, scroll down to the heading “Strain.”)
Ligaments and Tendons: Collagen-type fibres
Both ligaments and tendons are made up of pretty much the same stuff: very firm collagen-based cord-like structure. They change shape very little as you move since they must stabilise your joints and hold the bones steadily in place. They do not contract and cannot shorten (except over periods of months).
Muscle tissue: Myofibrils
Muscles, on the other hand, are incredibly pliable. They are made from softer, long, string-like cells called myofibrils. They need to flex and move as you do, so they are a lot more floppy. The muscles, not the ligaments or tendons, are what contract and shorten.
Fascia and Myofascia
Fascia wraps around every organ, bone, muscle, and even forms a layer under your skin in the body. You might have heard the term “myofascia.” Myofascia is the word we give only to the fascia that wraps around muscles.
Fascia holds the muscles in place like a kind of skin. It contains a small amount of contractile tissue (like muscle) but is primarily made out of collagen-like fibres (like ligaments and tendons). But fascia is very thin and flat instead of cord-like.
This thinness and flatness mean it can bend, warp, and flex along with the muscles it wraps around, but still holds a shape to which it returns. In this way, it takes the best parts of collagen and muscle tissue – strength and flexibility – and combines them.
Fascia also contains a LOT of sensory nerve endings, including pain receptors. In fact, your fascia contains more pain receptors than the muscle it wraps around! This makes it a sensory organ.
It is fascia that gives a muscle its shape. It is also fascia that holds a muscle together when it contracts with a lot of force. This stops the muscle from bursting out all over the place in a mess when it contracts.
Strains
When we talk about a “muscle,” we combine and include in that definition the muscle cells, the myofascia, and the tendon together. Any or all of these tissues can be injured or torn in a strain injury.
A strain injury involves tearing to some or all of the muscle mechanism.
The weakest part of the structure is the junction where muscle fibres transition and attach to its tendon fibres. This musculo-tendonous junction is the most common site of strain injuries.
Classifications of muscle strain injuries
You might have either a grade 1, grade 2 or grade 3 strain:
- Grade one tears are not very serious, and often just involve an over-stretching of the fibres. A bit like when you stretch a bed sheet and the fibres stretch but don’t break.
- A grade two tear is more serious. There are more fibres torn apart and there is often some deep bruising as blood vessels within the muscle also tear open.
- A grade three tear kind of sucks. A lot. The muscle and/or tendon is basically totally ruptured – severed all the way through. If you are unlucky enough to have a grade three tear, you’ll probably be out of action for a while.
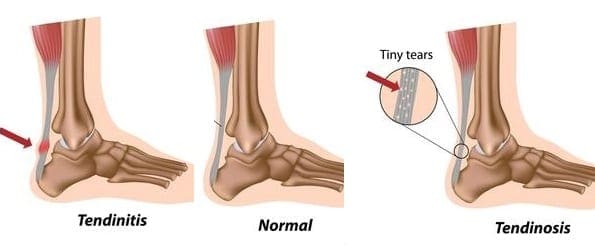
Tendinitis vs Tendinosis

What’s in a name?
The suffix ~itis means that the site of injury is inflamed. Signs of inflammation are redness, swelling, and heat in the local area around the injury. If these signs are not present, even if there is still pain, it cannot properly be defined as tendinitis.
Instead, it is defined as tendinosis, which is a degeneration, degradation, or tears in the tendon without inflammation. This can often happen in a tear injury older than about six weeks or so. Tendinosis injuries can be painful all the time, or only on specific movements.
Be careful with fresh or inflamed muscle strains
We need to take special care with an inflamed tendinitis injury so we don’t cause more damage. Re-injuring the muscle would be painful and slow down the healing process.[mfn]Some highly-trained therapists will intentionally re-injure a strain (or sprain, or other tissue) scar with the intention of then guiding the healing process from the beginning. This is a valid method but is only useful for the most stubborn or large scars. It is also quite painful.[/mfn]
With a tendinosis injury, on the other hand, we can go straight into full therapy.
Case study: Calf Muscle Strains
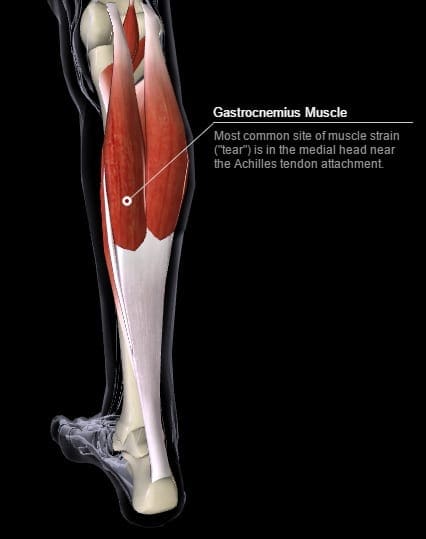
A common strain injury happens when you sprint off too quick from a standstill, and all your body weight goes suddenly through your gastrocnemius (calf, or gastroc) muscle as it contracts explosively. I’ve had clients tell me they did this by suddenly running for public transport.
In one of my cases recently the explosive movement through the muscle resulted in a grade one tear to the medial head of their gastrocnemius muscle. An ultrasound scan by a physiotherapist confirmed this.
Thankfully a muscle strain injury, especially an older, low-grade one, is one of the easiest injuries to resolve.
…BUT…
If you have a fresh strain injury less than a few days old, you need to rest.
- Anti-inflammatory analgesic medications or high-dose fish oil or curcumin may help to control your pain.
- Ice and compression may also help with pain and swelling if there is any.
- WAIT before getting it treated by a remedial massage therapist or another manual therapist. In the initial stages, we will only be able to help you relax the muscles around the injury, but not the injury itself.
- After a few days, only get treated by an experienced practitioner who properly assesses the strain before treating it. If a therapist treats you too aggressively, it may make your injury worse and your recovery more time-consuming – not to mention cause you unnecessary pain.
The road to recovery
If there is minimal pain, after a few days you can try moving the injury around like you normally would. Moving and stretching a healing strain injury is important to maintain function and flexibility. If a strain injury is kept still for too long, it may become stiff and cause other movement problems.
The key is not to over-do it! Getting good care and advice from a professional is the best way forward.
If you are experiencing increasing pain you must dial it back, get advice, and WAIT for it to start feeling better!
When the injury is settled, inflammation has gone, and there is pain only on movement and not when at rest, we can go forward with a scar tissue resolution protocol, as follows:
1. Release the muscle belly
In treatment we apply a technique called myofascial release, as well as compression broadening and deep cross-fibre gliding strokes to release the entire muscle belly and unload any pulling from muscle.
2. Test to isolate the injury
We then test the muscle under a light load – just enough to allow a pinpoint location of the site of injury. Usually you can point to the site of discomfort with one finger, as opposed to it being a wider area. This is especially true with older strains.
3. Multi-directional frictioning
Having located the site of injury, I apply moderate depth frictioning with the pads, not the tips, of my fingers for up to 30 seconds. This may hurt just a little, but should not be ‘painful’, per sé.
I apply the frictioning in multiple directions, after the multiple directions that your body lays down scar tissue in a cross-thatched way (to stabilise the site of injury). This softens (but does not realign) the scar tissue matrix.
4. Controlled resisted eccentric/concentric realignment
Once the collagen matrix has been softened, I help you through very lightly resisted muscle shortening and lengthening contractions. It is this movement that realigns the disorganised scar tissue into correctly oriented, organised, functional tissue.
5. Re-test to isolate remaining dysfunction
Then we re-test. If we can still find pain we do another pass of frictioning and resisted contractions. Most often the pain will decrease significantly with each pass.
In many cases, especially older injuries, we can completely resolve the pain and any discomfort in movement simply goes away. Many of my clients have said that “it is like magic.”
I like to reassure them that it is just biology! Although, I will admit it certainly looks like magic sometimes…!
Do you have an old, annoying strain injury? Book in now to come see me.
How NOT to treat a strain injury:
Footnotes:
